 As 2026 unfolds, state and federal lawmakers are increasingly treating oral health as part of larger health care conversations — especially around cost, access, workforce challenges, and public health.
As 2026 unfolds, state and federal lawmakers are increasingly treating oral health as part of larger health care conversations — especially around cost, access, workforce challenges, and public health.
Melissa Burroughs, Senior Director of Public Policy at CareQuest Institute, is watching a series of developments that could decide who gets the opportunity to access quality oral health care — and who will continue to face barriers. Below, she answers eight questions about what is shaping up to be the most critical time for oral health policy in decades.

Melissa Burroughs
Q: When you look ahead to 2026, what feels most urgent to address in oral health policy?
What feels most urgent is that oral health is being pulled into multiple policy conversations at once — public health, affordability, workforce, Medicaid, and even election politics. Decisions that may not seem “dental-specific,” like Medicaid work requirements or higher insurance premiums, can have outsized consequences for people’s ability to access dental care or improve their oral health. At the same time, there are very specific threats to oral health, like attacks on water fluoridation or efforts to scale back Medicaid dental benefits. Lawmakers need to understand this full picture, and how all of these issues can either exacerbate or help to improve our nation’s oral health crisis.
Q: Speaking of science, fluoride has been in the headlines more lately. What’s happening on the national and state levels?
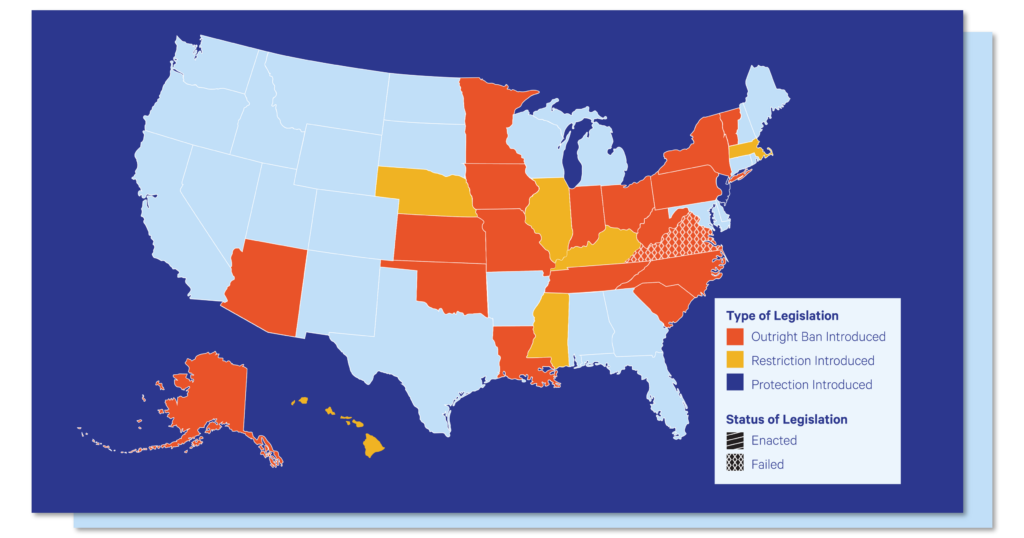
This map from CareQuest Institute shows the states considering legislation to restrict or ban fluoride in drinking water.
We’re seeing a new wave of state legislation aimed at restricting or banning community water fluoridation (CWF), alongside growing pressure on the US Environmental Protection Agency (EPA) to regulate fluoride. Right now, several states have introduced bills related to water fluoridation.
That matters because CWF is one of the most effective, evidence-based public health measures we have, especially for children and low-income communities. Rolling it back would increase rates of tooth decay and widen existing inequities.
Q: The federal government recently passed a law that will cut states’ Medicaid budgets. How does that affect access to oral health care?
Yes, states are facing serious budget pressure. And on top of those budget cuts, most states will also be implementing work-reporting requirements. Both trends put Medicaid dental coverage at risk. Adult dental benefits, which are optional under Medicaid, are often among the first items states cut in tight budgets. And if people lose their Medicaid because they can’t fulfill work-reporting requirements, they will lose their Medicaid health coverage and their dental coverage.
We’re closely monitoring states like California, Colorado, Idaho, and Massachusetts, as well as Washington, D.C., as places where specific proposals to cut benefits are under consideration. The reality is that millions of people rely on Medicaid for dental care; losing that coverage often means patients with oral health problems will delay getting care until it becomes an emergency.
Q: Many states are focusing on dental therapy, too. What are dental therapists, and what could we see as far as legislation in 2026?
Dental therapy is a newer profession that can improve access to routine, affordable oral health care — particularly in rural, underserved, and low-income communities. Dental therapists are licensed, mid-level providers, similar to physician assistants in medicine. They work under a dentist’s supervision and provide preventive and restorative care such as fillings, simple extractions, exams, and temporary crowns.
In 2026, we could see major legislative movement to authorize dental therapy in large states like Florida, Massachusetts, and New York. This would be a game changer for access to care and workforce capacity in those states.
Q: How could changes to the Affordable Care Act marketplace health insurance affect dental coverage?
With Congress appearing unlikely to extend enhanced premium tax credits, which make health insurance premiums more affordable, we’re concerned that rising premiums will squeeze household budgets even further. When that happens, standalone dental coverage is often one of the first benefits people drop.
That creates a ripple effect as people skip preventive care, problems worsen, and eventually they end up in emergency rooms for issues that could have been treated earlier and more affordably.
Q: With midterms coming up, where does dental care fit into the political conversation?
Dental care isn’t always front and center in election coverage, but it’s absolutely part of the broader affordability conversation voters and policymakers are having. The cost of care, the cost of insurance premiums, and health care workforce shortages also determine whether people can get the access to dental care they need.
As affordability becomes a defining issue in the midterms, oral health will have a seat at the table.
Q: Are there any government programs that make you optimistic about the future?
Yes! Oral health projects in some states’ Rural Health Transformation Grants give me hope. New federal investments have the potential to improve rural oral health infrastructure where states prioritize it. We’re seeing some promising early trends, and if those investments are sustained, they could help close long-standing access gaps.
Also, there’s growing bipartisan support on Capitol Hill to improve veterans’ access to care. Lawmakers are increasingly recognizing that oral health is essential to overall health — and that veterans need solutions.
Currently, US Veterans Affairs (VA) dental coverage is limited to veterans who have service-connected dental conditions, are former prisoners of war, or are 100% disabled. That leaves about 80% of veterans without dental benefits through the VA.
Q: What is the most important message you want policymakers to understand in 2026?
Oral health isn’t separate from health care; it’s foundational to it. When policies undermine access to dental care, people don’t just lose dental cleanings or fillings; they lose their ability to eat, work, learn, and stay healthy. The reverse is true when policymakers invest in oral health: It can benefit overall health, save constituents money, and improve the health care system. The choices policymakers make in 2026 will have real, long-term oral health impacts for millions of people.
